Neuro (Brain)
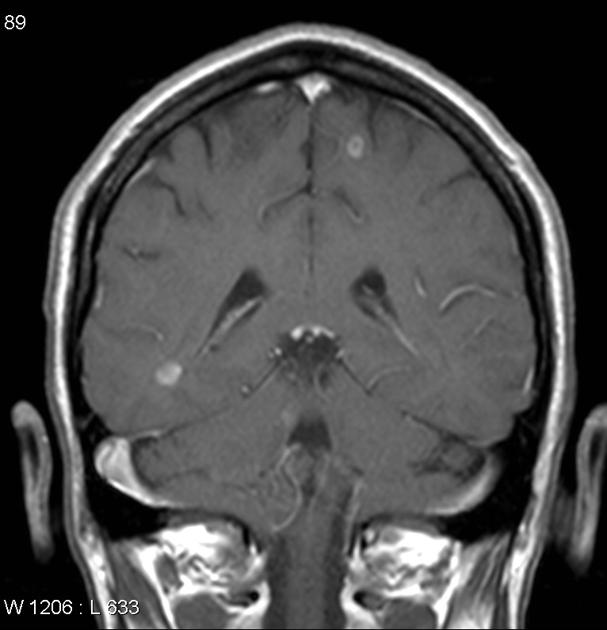
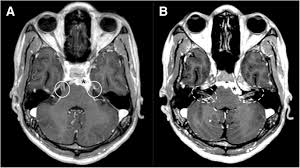
Neurosarcoidosis is a rare but serious form of sarcoidosis that affects the brain, spinal cord, and peripheral nerves. It occurs when inflammatory clusters called granulomas form in nervous system tissue, disrupting normal neurological function. Although only about 5–15% of people with sarcoidosis develop neurosarcoidosis, its symptoms can be life-altering and often require specialized care.
What Causes Neurosarcoidosis?
The exact cause is unknown, but neurosarcoidosis is believed to result from an overactive immune response that causes inflammation in the nervous system. It may occur:
- In people with existing sarcoidosis (lungs, lymph nodes, skin, eyes, etc.)
- As the first or only sign of sarcoidosis (which makes diagnosis more challenging)
Parts of the Nervous System Affected
Neurosarcoidosis can involve:
- Brain (meninges, pituitary gland, hypothalamus)
- Spinal cord
- Cranial nerves (especially facial and optic nerves)
- Peripheral nerves
- Autonomic nervous system (controls heart rate, digestion, blood pressure)
Common Symptoms
Symptoms vary widely depending on which area is affected and may appear suddenly or progress slowly.
Brain-Related Symptoms
- Chronic or severe headaches
- Seizures
- Memory problems or confusion
- Personality or mood changes
- Difficulty concentrating
- Sleep disturbances
Cranial Nerve Symptoms
- Facial paralysis (Bell’s palsy–like symptoms)
- Vision loss or blurred vision
- Hearing loss or ringing in the ears
- Difficulty swallowing or speaking
Spinal Cord & Nerve Symptoms
- Weakness in arms or legs
- Numbness or tingling
- Balance and coordination problems
- Chronic pain or nerve pain
- Loss of bladder or bowel control
Hormonal & Autonomic Symptoms
(when the pituitary or hypothalamus is involved)
- Extreme fatigue
- Abnormal thirst or urination
- Temperature regulation problems
- Sexual dysfunction
- Blood pressure or heart rate irregularities
How Neurosarcoidosis Is Diagnosed
Diagnosis is often complex and usually involves multiple tests, as symptoms can mimic other neurological conditions like MS or lupus.
Common diagnostic tools include:
- MRI of the brain and spinal cord (with contrast)
- Lumbar puncture (spinal tap) to examine cerebrospinal fluid
- Blood tests to assess inflammation and rule out infections
- PET scans to detect active inflammation
- Biopsy (when accessible tissue is available)
- Review of existing sarcoidosis history
Treatment Options
There is no cure, but treatment focuses on reducing inflammation, managing symptoms, and preventing permanent nerve damage.
Medical Treatments
- Corticosteroids (Prednisone) – first-line treatment
- Immunosuppressive medications (methotrexate, azathioprine, mycophenolate)
- Biologic therapies (such as TNF-alpha inhibitors) for severe or resistant cases
Supportive & Symptom Management
- Anti-seizure medications
- Pain management for neuropathy
- Hormone replacement therapy (if pituitary affected)
- Physical, occupational, or speech therapy
Lifestyle & Holistic Support (Complementary)
While not a replacement for medical treatment, many patients benefit from supportive approaches:
- Anti-inflammatory nutrition
- Gentle movement and physical therapy
- Stress management (prayer, meditation, breathwork)
- Adequate rest and pacing to manage fatigue
- Emotional and mental health support
⚠️ Always consult a healthcare provider before starting supplements or alternative therapies.
Prognosis & Quality of Life
Neurosarcoidosis can be chronic and relapsing, but many people experience symptom improvement with early and consistent treatment. Outcomes depend on:
- Severity and location of inflammation
- Speed of diagnosis
- Response to treatment
- Ongoing monitoring and lifestyle support
Some individuals achieve remission, while others may need long-term management.
Living With Neurosarcoidosis
Living with neurosarcoidosis often requires:
- A neurologist and sarcoidosis specialist
- Ongoing imaging and symptom tracking
- Strong self-advocacy and education
- Faith, community, and emotional support
You are not weak for needing rest, help, or hope—your journey matters.
Faith-Centered Encouragement
“The Lord is close to the brokenhearted and saves those who are crushed in spirit.” — Psalm 34:18
Even in neurological struggles, strength, healing, and peace are still possible—one step, one prayer, one day at a time.