Cutaneous (Skin)
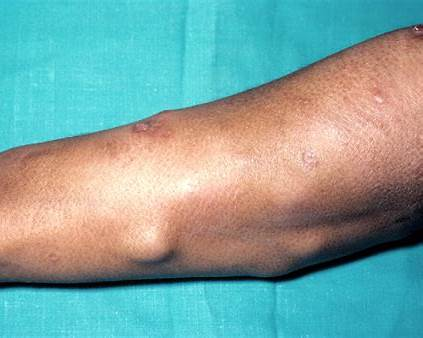
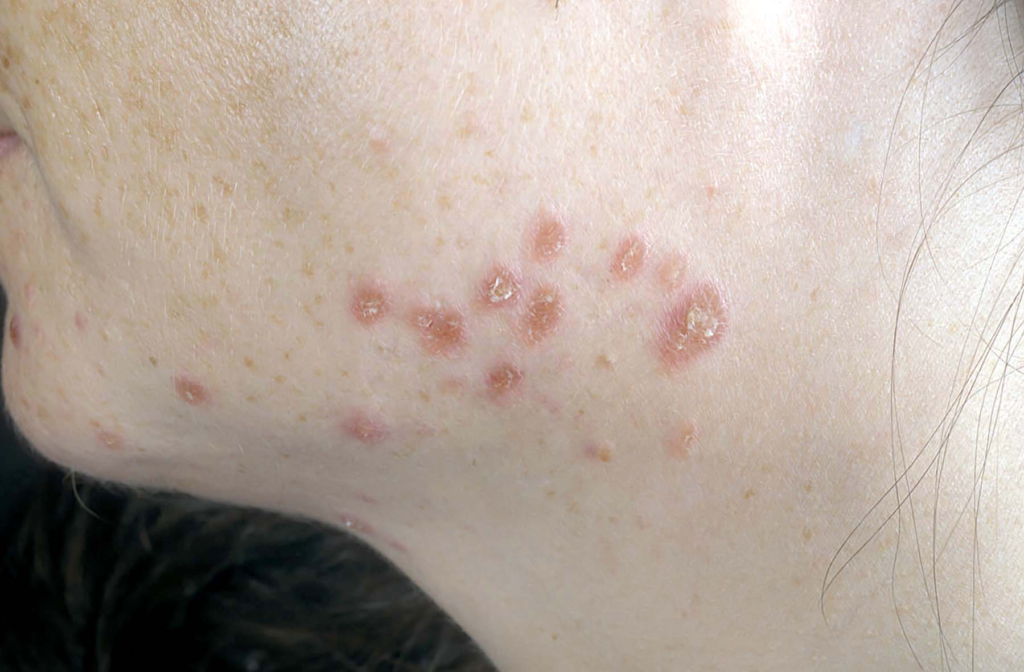
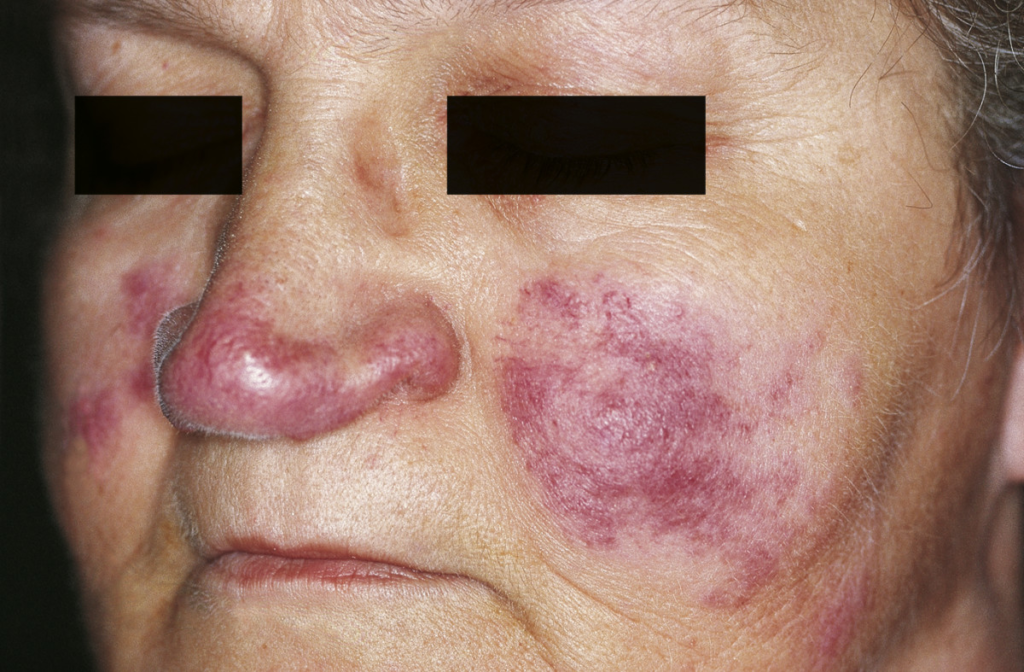
Cutaneous sarcoidosis is a form of sarcoidosis that affects the skin, occurring in about 25–35% of people living with the condition. It develops when clusters of inflammatory cells called granulomas form in the skin. Skin involvement may appear on its own or alongside sarcoidosis affecting the lungs, lymph nodes, eyes, or other organs.
Skin sarcoidosis can vary greatly in appearance and severity—from mild cosmetic changes to painful or disfiguring lesions—and often provides early clues to an underlying systemic condition.
Common Signs & Symptoms
Cutaneous sarcoidosis can look very different from person to person. Lesions may appear anywhere on the body but are most commonly found on the face, neck, arms, legs, scalp, and torso.
Typical symptoms include:
- Red, purple, brown, or flesh-colored lesions
- Raised bumps or plaques
- Rashes that do not itch or scale
- Skin thickening or nodules
- Tender or painful lumps (especially on the legs)
- Changes in skin texture or color
- Lesions that worsen with sun exposure
⚠️ Important: Skin sarcoidosis is often not itchy, which helps distinguish it from eczema, psoriasis, or allergic rashes.
Types of Cutaneous Sarcoidosis
1. Papular Sarcoidosis
- Small, raised bumps (papules)
- Often found on the face, eyelids, lips, and neck
- May be skin-colored, red, or purple
- More common in early disease
2. Plaque Sarcoidosis
- Larger, flat, thickened patches
- Often chronic and persistent
- Can leave long-term discoloration or scarring
3. Lupus Pernio
- Chronic, bluish-purple discoloration
- Commonly affects the nose, cheeks, lips, and ears
- Associated with more severe or long-standing disease
- Can cause facial disfigurement if untreated
4. Erythema Nodosum
- Painful, red, tender nodules—usually on the shins
- Often accompanied by fever, joint pain, and fatigue
- More common in women
- Typically indicates acute sarcoidosis and often resolves on its own
5. Nodular Sarcoidosis
- Firm lumps beneath the skin
- May resemble cysts or tumors
- Usually painless but noticeable
6. Scar or Tattoo Sarcoidosis
- Granulomas form in old scars or tattoos
- Areas may swell, darken, or become raised
- Can be a key diagnostic clue
What Causes Skin Sarcoidosis?
The exact cause is unknown, but experts believe cutaneous sarcoidosis is related to:
- An overactive immune response
- Genetic susceptibility
- Environmental or infectious triggers
The immune system mistakenly forms granulomas in the skin, even when no infection is present.
Diagnosis
Diagnosis often involves:
- Skin biopsy (most definitive test)
- Blood tests (inflammatory markers, calcium levels)
- Chest imaging to check for lung involvement
- Eye exams or other organ screening if systemic disease is suspected
Because skin sarcoidosis can mimic other skin conditions, biopsy is critical for accurate diagnosis.
Treatment Options
Treatment depends on severity, symptoms, and whether other organs are involved.
Medical Treatments
- Topical corticosteroids (for mild disease)
- Corticosteroid injections into lesions
- Oral corticosteroids (for widespread or severe cases)
- Immunosuppressive medications (methotrexate, hydroxychloroquine)
- Biologic therapies in resistant cases
Supportive & Lifestyle Care
- Sun protection (UV exposure can worsen lesions)
- Gentle skincare routines
- Anti-inflammatory nutrition
- Stress management (stress can trigger flares)
⚠️ Always work with a healthcare provider—especially a dermatologist or sarcoidosis specialist—to determine the safest treatment plan.
Emotional & Quality of Life Impact
Skin sarcoidosis can significantly affect:
- Self-esteem and body image
- Emotional well-being
- Social confidence
- Mental health (especially when facial lesions are present)
Support groups, counseling, and faith-based encouragement can play an important role in healing and resilience.
Faith & Encouragement
Living with visible symptoms can be emotionally heavy. Remember:
“The Lord is close to the brokenhearted and saves those who are crushed in spirit.” — Psalm 34:18
You are not defined by your diagnosis or appearance. Healing is not only physical—it is emotional, mental, and spiritual.
When to See a Doctor
- New or worsening skin lesions
- Facial swelling or discoloration
- Painful nodules on the legs
- Skin changes along with fatigue, shortness of breath, or vision changes
Early care can prevent complications and improve outcomes.