Pulmonary (Lungs)
Different Types of Sarcoidosis & How They Affect the Body
Sarcoidosis is a complex inflammatory disease that can affect multiple organs and systems in the body. It occurs when clusters of inflammatory cells, called granulomas, form in tissues and organs. While sarcoidosis most commonly affects the lungs, it is a systemic condition, meaning it can impact many areas of the body—sometimes all at once.
Understanding the different types of sarcoidosis can help patients recognize symptoms early, seek appropriate care, and better manage daily life with this condition.
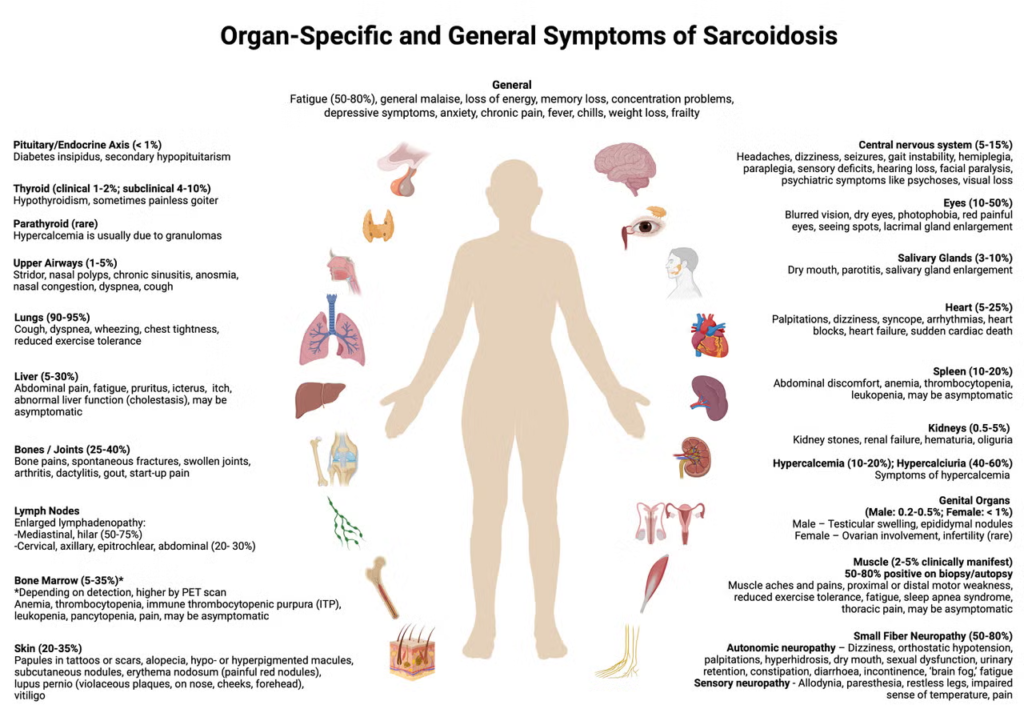
Pulmonary sarcoidosis is the most common form of sarcoidosis, affecting the lungs and nearby lymph nodes. For many people, it is the first—and sometimes only—organ system involved. This page provides a clear, compassionate, and medically grounded overview to help patients, caregivers, and families understand what pulmonary sarcoidosis is, how it affects the body, and how it’s managed over time.
What Is Pulmonary Sarcoidosis?
Pulmonary sarcoidosis is an inflammatory condition in which clusters of immune cells, called granulomas, form in the lungs. These granulomas can interfere with normal lung function, affecting breathing and oxygen exchange.
While some people experience mild symptoms—or none at all—others may develop chronic or progressive lung disease that requires ongoing care.
Why the Lungs Are Commonly Affected
The lungs are constantly exposed to environmental triggers such as dust, chemicals, bacteria, and viruses. In people with sarcoidosis, the immune system may overreact to a trigger, causing persistent inflammation and granuloma formation.
The exact cause is still unknown, but research suggests a combination of:
- Genetic susceptibility
- Environmental or occupational exposure
- Immune system dysregulation
Common Symptoms of Pulmonary Sarcoidosis
Symptoms vary widely. Some individuals are diagnosed after an abnormal chest X-ray, while others experience significant respiratory distress.
Respiratory Symptoms
- Persistent dry cough
- Shortness of breath (especially with exertion)
- Chest tightness or pain
- Wheezing
- Reduced exercise tolerance
Systemic (Whole-Body) Symptoms
- Fatigue or exhaustion
- Fever or night sweats
- Unexplained weight loss
- General weakness
Important: Symptoms do not always match disease severity. Some people with extensive lung involvement feel relatively well, while others with mild imaging changes may feel very ill.
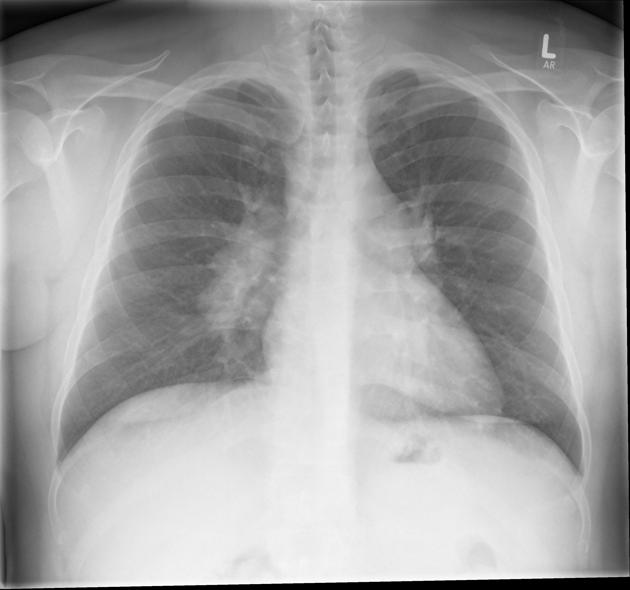
Stages of Pulmonary Sarcoidosis (Chest Imaging)
Pulmonary sarcoidosis is often classified into stages based on chest X-ray findings (not disease severity):
- Stage 0: Normal chest X-ray
- Stage I: Enlarged lymph nodes in the chest (hilar adenopathy)
- Stage II: Lymph node enlargement + lung infiltrates
- Stage III: Lung infiltrates without lymph node enlargement
- Stage IV: Pulmonary fibrosis (permanent lung scarring)
Not everyone progresses through all stages, and many people improve or go into remission.
How Pulmonary Sarcoidosis Is Diagnosed
Diagnosis usually involves multiple tests, as no single test confirms sarcoidosis.
Common Diagnostic Tools
- Chest X-ray
- High-resolution CT scan
- Pulmonary function tests (PFTs)
- Blood tests (inflammatory markers, calcium levels)
- Bronchoscopy with biopsy (to confirm granulomas)
- Exclusion of infections or other lung diseases
Pulmonary Function Tests: What They Show
Pulmonary function tests help assess:
- Lung volume
- Airflow
- Oxygen exchange
Pulmonary sarcoidosis may cause:
- Restrictive lung disease
- Reduced diffusion capacity (DLCO)
- Exercise-related oxygen drops
Regular testing helps track disease progression and treatment response.
Treatment Options for Pulmonary Sarcoidosis
Not everyone with pulmonary sarcoidosis needs medication. Treatment depends on:
- Symptom severity
- Lung function changes
- Imaging progression
- Impact on quality of life
Conventional Medical Treatments
- Corticosteroids (e.g., prednisone): First-line therapy
- Steroid-sparing agents: Methotrexate, azathioprine, or similar medications
- Biologic therapies: For severe or refractory disease
Supportive & Lifestyle Care
- Pulmonary rehabilitation
- Gentle, regular exercise
- Anti-inflammatory nutrition
- Stress reduction and sleep support
- Avoidance of lung irritants (smoke, chemicals)
Can Pulmonary Sarcoidosis Go Into Remission?
Yes. Many people experience:
- Spontaneous remission (especially early-stage disease)
- Long-term stability with monitoring
- Improvement with treatment
However, some develop chronic pulmonary sarcoidosis, requiring ongoing management.
Potential Complications
If left untreated or poorly controlled, pulmonary sarcoidosis may lead to:
- Pulmonary fibrosis (lung scarring)
- Chronic respiratory insufficiency
- Pulmonary hypertension
- Increased risk of infections
Early monitoring and personalized care are key to reducing complications.
Living Well With Pulmonary Sarcoidosis
Living with pulmonary sarcoidosis is not just about managing symptoms—it’s about preserving hope, strength, and quality of life.
Helpful strategies include:
- Building a trusted medical team
- Tracking symptoms and triggers
- Practicing energy conservation
- Seeking emotional and faith-based support
- Connecting with others who understand the journey
You are not weak for needing rest. You are not failing because your body needs care. Healing is not linear—and you are not alone.
When to Seek Medical Help Urgently
Contact a healthcare provider if you experience:
- Sudden worsening shortness of breath
- Chest pain not related to coughing
- New oxygen needs
- Fainting or severe fatigue
Final Thoughts
Pulmonary sarcoidosis affects each person differently, but knowledge empowers advocacy. With early detection, thoughtful treatment, and whole-person support, many people live full, meaningful lives despite this condition.